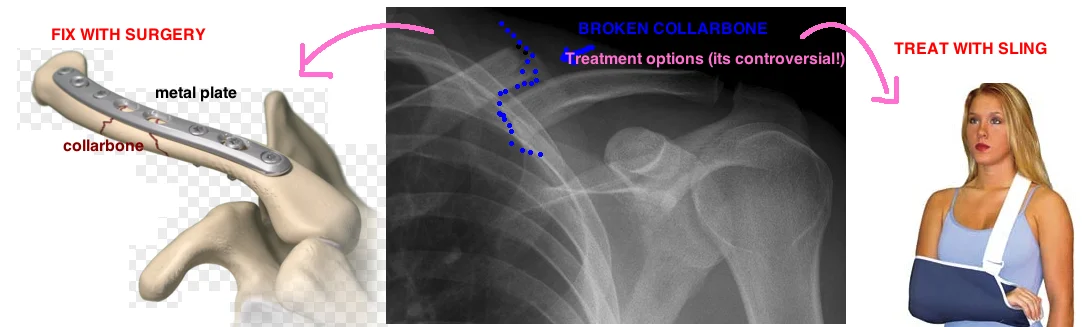
How are orthopedic surgeons treating broken clavicles in 2015?
Before we get into it, lets quickly review the history of broken collarbones. A broken collarbone (aka clavicle fracture) is one of the most common injuries seen by an orthopedic surgeon. 30 years ago these injuries were universally treated without surgery (unless the bone was sticking out of the skin). Patients were given a sling for a few weeks and sent on their way. Now doctors aren't so sure that non-surgical management is the best treatment. About 85% heal without major issues. About 15% don't completely heal. A lot of broken collarbones that fail to heal never actually cause symptoms. But, some broken collarbones remain painful, and prevent normal return of function. Doctors have found some ways to predict which collarbones are at risk for causing pain many months later, and studies show that surgery is an effect way to treat collarbones that remain painful. See our discussion of clavicle fractures for a full overview.
But the controversy remains. Old doctors grew up learning from Dr. Neer that "all clavicle fractures" heal very well (see reference). Young doctors don't trust those old studies, and they look to newer studies that say surgery is sometimes a better treatment (see reference). So what are orthopedic surgeons doing these days with broken collarbones?
A recent study looked at patients in Florida with clavicle fractures in the year 2010. I looks like 95% of broken collarbones are being treated without surgery. So even though around the country, the number of surgeries for a broken clavicle as increased 63% (from 2007 to 2013), the vast majority of cases are still treated with a sling and followed every few weeks with an x-ray.
Interestingly, the INSURANCE of the patient had a significant effect on treatment. This is a little discouraging to hear because you never want financial factors to influence medical care. You want people to get surgery or get a sling because its the best treatment. However, it was found that the 5% of people getting surgery were 7x more likely to have private insurance than Medicare, Medicaid or no insurance ("self pay").
References.
1) Bliss RL, Mora AM, Krause PC. Does Insurance Status Affect the Management of Acute Clavicle Fractures? J Orthop Trauma. 2016 May;30(5):269-72. insurance affects surgical indication. read full article.
2) Neer C.S.: Nonunion of the clavicle. J Am Med Assoc 1960; 172: pp. 1006-1011. original article on clavicle fractures indicating only 1% nonunion risk. full article.
3) Rowe C.R.: An atlas of anatomy and treatment of midclavicular fractures. Clin Orthop Relat Res 1968; 58: pp. 29-42. another older article on clavicle fractures indicating very low nonunion risk. full article.
4) Robinson C.M., Court-Brown C.M., McQueen M.M., and Wakefield A.E.: Estimating the risk of nonunion following nonoperative treatment of a clavicular fracture. J Bone Joint Surg Am 2004; 86: pp. 1359-1365. modern version of older studies highlighting good outcomes with nonoperative management (slightly higher than original papers, 4.5%). full article.
5) Nonoperative treatment compared with plate fixation of displaced midshaft clavicle fractures. A multicenter, randomized clinical trial. J Bone Joint Surg Am 2007; 89: pp. 1-10. New study showing better functional outcomes with surgical fixation. game changer paper. see full article.
6) Hill J.M., McGuire M.H., and Crosby L.A.: Closed treatment of displaced middle-third fractures of the clavicle gives poor results. J Bone Joint Surg Br 1997; 79: pp. 537-539. 15% nonunion rate in displaced fractures, 30% poor result. classic paper. see full article.
8) Leroux T., Wasserstein D., Henry P., Khoshbin A., Dwyer T., Ogilvie-Harris D., et al: Rate of and risk factors for reoperation after open reduction and internal fixation of midshaft clavicle fractures: a population-based study in Ontario, Canada. J Bone Joint Surg Am 2014; 96: pp. 1119-1125. Studies reporting high re-operation rates for plate removal (18-24%), see full article. However, recent paper suggests this is only 10-14%, although standard plate vs. contoured plate makes no difference. Naimark M. et al. Plate fixation of midshaft clavicular fractures: patient-reported outcomes and hardware-related complications. J Shoulder Elbow Surg. 2016 May;25(5):739-46. see full article.